
Background
Personality, according to the American Psychological Association, refers to “individual differences in characteristic patterns of thinking, feeling, and behaving’. In short, it’s what makes us us, what makes me different from you. It shapes how we process and understand our individual lives and all the nuances they bring, and in turn those experiences also shape our personality.
Though it may have seemed obvious, there have been recent findings that personality could play a larger role than we may have thought in determining an individual’s health. For example, Youyou et al found computer-based personality judgements could predict an individual’s physical health or even if they’re more prone to substance use (Youyou et al 2015).
This leads to a recent study by Kim et al who examined the correlations between personality and gut-microbiome composition, in other words the bacteria we host in our intestines (Kim et al 2018). But why bacteria, and how does this relate to personality?
Recently there has been a lot of evidence showing that bacteria, especially in the gut, can influence a multitude of physiological aspects in our bodies. For example, Allen et al expounded on the relationship between our brains, our gastrointestinal tracts, and the microbiota that are contained there (Allen et al 2017). What used to be known as the gut-brain axis is now being realized as a three-way system also involving our microflora.
This brings us back to our original study of interest with Kim et al. They realized that personalities are important, it’s a driving force behind our behavioral patterns and can be associated with not only our physical health but different neurological disorders as well, such as Alzheimer’s or depression. But they also realized the importance of the gut microbiome and how closely it’s linked to our brain. So then they asked:
Is there a correlation between the human gut microbiome and personality? And if so, what is it?
Their hypothesis was there would indeed be a correlation between different personalities and microbiome composition.
Evidence
For this study, they first needed people. A lot of people.
Fortunately, Kim et al are based in South Korea, and were able to use a cohort (672 people) of healthy Korean men and women already undergoing comprehensive annual check ups. For this study, they also filled out a 240-item questionnaire on their personality. The aim of the test was to closely examine an individual’s Big Five personality traits: openness to experience (inventive and curious), conscientiousness (organized and dependable), extraversion (outgoing and energetic), agreeableness (compassionate and cooperative), and neuroticism (sensitive and nervous).
Using stool samples from the participants, they identified the bacteria by analyzing their unique gene sequences and matched it with existing sequence databases. Then they exacted correlations between different gut microbiota and an individual’s results on the personality exam.
To find correlations between personality and gut microbiome, they focused on the individual relationships between each trait and different bacterial compositions. What they found confirmed their hypothesis: there is a correlation between gut microbiome composition and the differing personality traits. Though they found many different correlations, their key findings are as follows:
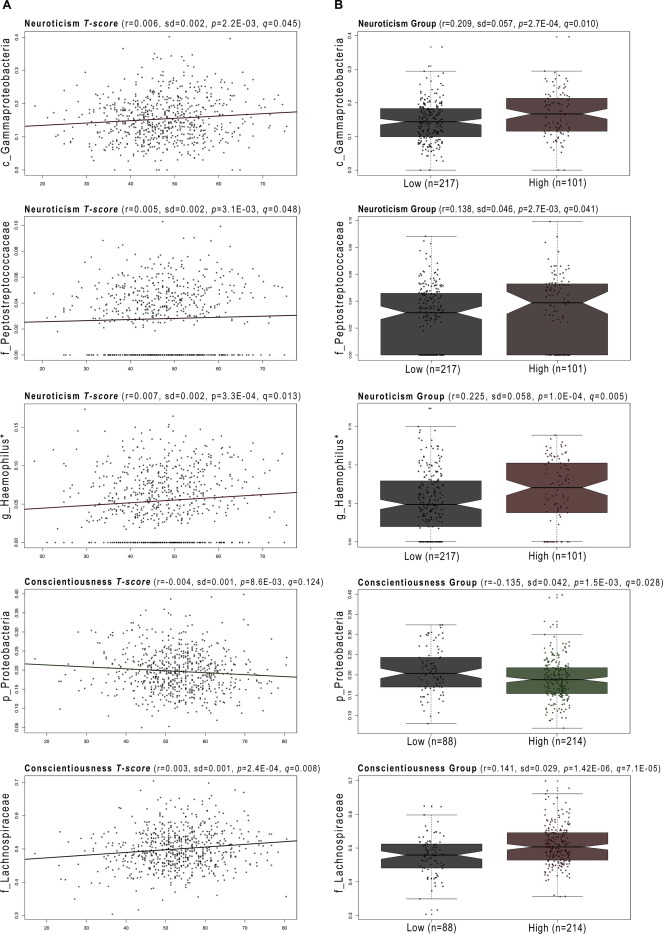
- High neuroticism correlates with high abundance of Gammaproteobacteria
- Low conscientiousness correlates with high abundance of Proteobacteria
- High conscientiousness correlates with increased abundance of Lachnospiraceae
- Branched-chain amino acid (BCAA) degradation pathways correlate with high neuroticism
To possibly explain these correlations, Kim et al first stated the association between neuroticism and conscientiousness with increased morbidity and mortality. According to another personality study by Goodwin and Friedman using the Big Five traits, they found that neurotic individuals or individuals low in conscientiousness tend to have more chronic illnesses (Goodwin et al 2006). It just so happens that the key findings in Kim et al’s study revolves around these two personality traits.
Kim et al explain that the degradation of BCAAs is important for contributing ATP (a common molecule inferring biochemical energy; think of it as our body’s energy currency) to Proteobacteria. This could elucidate the relationship between enriched BCAA degradation pathways and high abundance of Gammaproteobacteria in high neuroticism. But to further expound on these correlations, Kim et al relate their findings to one of the most important ways our body deals with stress: inflammation.
Unfortunately, inflammation is complicated. Most of the time it’s an advantageous mechanism our bodies employ to increase the rate of repair at the site of damage but too much of inflammation (chronic inflammation) can be fatal as seen in autoimmune disorders. Kim et al reference studies that posit correlations between neuroticism and conscientiousness with greater circulation of inflammatory markers (Luchetii et al 2014, Sutin et al 2010). They also reference another study that states the importance of Lachnospiraceae and other butyrate-producing bacteria in anti-inflammatory mechanisms (Machiels et al 2014).
I think it’s important to state that Kim et al’s study was not intended to examine the mechanistic relationships between the pronounced bacteria and their correlated personality traits. Their study was not designed to answer causality between the two. What they did find though was important and provides the foundation for future studies that do examine the mechanistic and potentially causal relationships between gut microbiome, personality traits, and ultimately, human health.
Future Experiments
Now that there has been evidence laid forth that personality is correlated with gut microbial composition, I think the next step would be look closer at the relationship between the two, specifically in determining any causality or determining the mechanisms of how they affect each other. For example, subjecting mouse models to Gammaproteobacteria or another elevated group of bacteria found in this study. Once the mouse has undergone the change, we could then wait for a potentially resulting effect.
In this study, all of the participants were Korean. Different cultures have varying diets which can potentially play a large role in determining microbiome composition. A study by Clayton et al suggested that diet, especially Westernized diets, can change the gut microbiome in nonhuman primates (Clayton et al 2016). In a sense, having an all Korean population was beneficial in minimizing differences and determining the personality-microbiome relationship for one geographically and culturally distinct group of people. However if we were to provide more context in these relationships with the world at large, a multicultural study would be necessary.
More Information
Kim et al’s previous studies on the genetic and biologic link between mental health and personality: 1, 2.
A short video on the basics of the Big Five personalities from the Youtube channel “Seeker’.
References
- “Personality.’ American Psychological Association, American Psychological Association, www.apa.org/topics/personality/.
- Youyou W, Kosinski M, Stillwell D. Computer-based personality judgments are more accurate than those made by humans. Proc Natl Acad Sci USA. 2015;112(4):1036-40.
- Kim HN, Yun Y, Ryu S, et al. Correlation between gut microbiota and personality in adults: A cross-sectional study. Brain Behav Immun. 2018;69:374-385.
- Allen AP, Dinan TG, Clarke G, Cryan JF. A psychology of the human brain-gut-microbiome axis. Soc Personal Psychol Compass. 2017;11(4):e12309.
- Mccrae RR, Costa PT, Martin TA. The NEO-PI-3: a more readable revised NEO Personality Inventory. J Pers Assess. 2005;84(3):261-70.
- Goodwin RD, Friedman HS. Health status and the five-factor personality traits in a nationally representative sample. J Health Psychol. 2006;11(5):643-54.
- Luchetti M, Barkley JM, Stephan Y, Terracciano A, Sutin AR. Five-factor model personality traits and inflammatory markers: new data and a meta-analysis. Psychoneuroendocrinology. 2014;50:181-93.
- Sutin AR, Terracciano A, Deiana B, et al. High neuroticism and low conscientiousness are associated with interleukin-6. Psychol Med. 2010;40(9):1485-93.
- Machiels K, Joossens M, Sabino J, et al. A decrease of the butyrate-producing species Roseburia hominis and Faecalibacterium prausnitzii defines dysbiosis in patients with ulcerative colitis. Gut. 2014;63(8):1275-83.
- Clayton JB, Vangay P, Huang H, et al. Captivity humanizes the primate microbiome. Proc Natl Acad Sci USA. 2016;113(37):10376-81.
