When studying mental illness, the brain has long been the focal organ of interest. Psychiatry and neurobiology examine communication from the brain and how its chemical imbalance produces central nervous system (CNS) disorders such as depression and anxiety. However, microbiology presents a new avenue of inquiry that is looking from the opposite direction: how is communication to the brain affecting mental health? This is a provocative question under investigation through recent studies of the microbiota of our gut.
Gut-brain axis
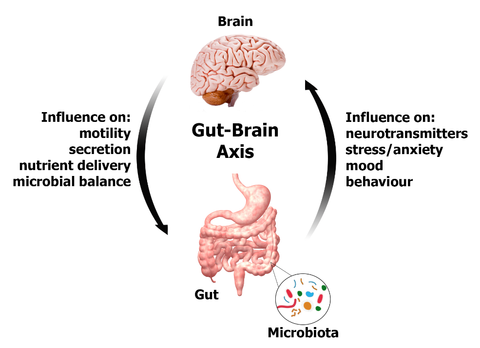
The gut-brain axis describes the bidirectional communication pathway between our brain and the millions of microbes inhabiting our gut. Our gut not only responds to signals from the brain, but also influences brain function in return (Dinan et al., 2015). The number of microbes is about 100-fold of our own genes and the microbiota in the gut weigh about as much as our brain (Dinan and Cryan, 2016) Studies have shown that manipulating microbial compositions can have as much of an effect on behavior as directly manipulating chemicals in the brain. For example, in animal and preclinical human trial administering probiotic species of Lactobacillus and Bifidobacterium reduced anxious and depressive behaviors comparable to the effect of pharmaceutical antidepressants (Bravo et al., 2011; Desbonnet et al., 2010; Benton et al., 2006; Rao et al., 2009). These studies have suggested probiotics as an alternative treatment therapy for anxiety and depression disorders.
Cognitive reactivity to sad mood
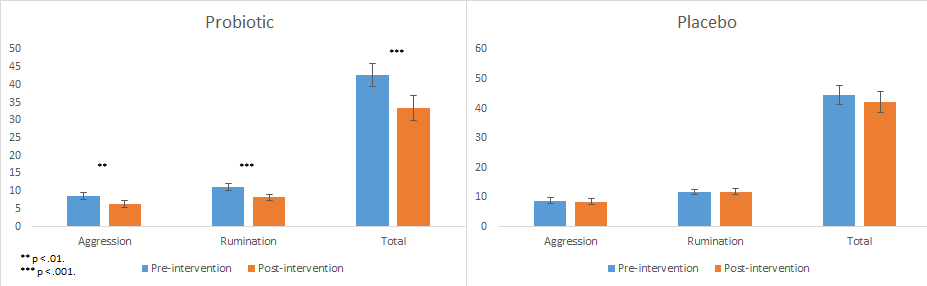
Treating CNS disorders is excellent, but could manipulating our gut microbes possibly serve as a preventative strategy? Laura Steenbergen and her colleagues at Leiden University in the Netherlands wanted to see if sad mood could be improved by probiotics in people without innate anxiety or depression (Steenbergen et al., 2015). To test this, 40 mentally healthy individuals, not suffering from or having family history of mental illness, were screened to participate in a 4-week probiotic intervention. The participants were randomly assigned so that half received the multi-species probiotic and the other half received a placebo to see if this intervention really worked. The probiotic and placebo treatments looked identical and the participants were not aware of the placebo treatment. They then went through an initial survey to establish symptoms of depression and anxiety as well as cognitive reactivity to sad mood. Cognitive reactivity refers to the vulnerability to depression characterized by ruminative thoughts (thinking about possible causes and consequences of actions and what you could have changed to prevent present emotional discomfort), aggression, hopelessness and suicidal thoughts. The survey was retaken at the end of the probiotic treatment and the pre and post-intervention surveys were compared to see how the probiotic effected thoughts associated with sad mood. Compared to placebo controls, participants who received the probiotic treatment reported less reactivity to sad mood, specifically in aggression and rumination (Fig 1). When persistent, ruminative and aggressive thoughts are predictive of depressive episodes and suicidal ideation. This effect was more pronounced in individuals who showed higher reactivity from the baseline in the initial questionnaire, which is in line with other studies that have reported a probiotic effect on depression that was not significantly detected in controls (Benton et al., 2006). Because these were mentally healthy individuals the results are not confounded by depressive predisposition, but instead illustrate what probiotics can do to improve personal disposition when in a sad mood as a preventative strategy of depressive episodes.
Probiotics as the next ‘happy pill?’
Probiotics seem to show the most pronounced effect in those already suffering from depressive behaviors, but also shows an ability to improve mood. In this light, it seems that probiotic intervention would provide best as a treatment therapy for central nervous system disorders. For those who are mentally healthy, probiotics seem to improve ability to not dwell on sad thoughts and could serve as a general mood enhancer to prevent developing depression. However, dependence on a probiotic intervention does not establish a healthy gut capable of sustainably producing appropriate signals to the brain. Diet has a profound effect on the microbiome. High fat diets have been shown to increase anxiety and depressive behaviors and this effect is not rescued by exercise alone (Kang et al., 2014). Presumably, probiotics will not undermine the effect of diet, so it would be advantageous to study probiotics in conjunction with diet to see how we can improve our microbiome at its core.
Supplement or stabilize?
Our bodies are as much microbe as they are us and they play a key role in our physiology. It is apparent that there is a much bigger picture that influences behavior than our brain alone. Probiotics could potentially replace the need for pharmaceutical interventions that are highly symptomatic and only provide temporary relief from psychological distress. Instead of synthesizing neurotransmitters and neuromodulators, we can employ the natural capacity of microbes to produce those important chemicals that signal appropriate functions in the brain. In this light, it would be interesting to study the gut-brain axis in terms of happy mood. Could microbes possibly play a role in modulating chemicals such as serotonin or dopamine to the brain? Might microbes not only reduce reactivity to sad mood, but possibly induce happy mood?
Probiotics are opening the door for a whole new approach to human health. However, I don’t suggest picking up a probiotic supplement on your next trip to the grocery store to help keep you chipper. More research needs to be done to provide more than correlations, so that we can better understand the specific functions and pathways that microbes influence. We need to figure out what to provide our bodies with to foster a healthy microbiome so that the communication scaffolding that our body uses to talk to itself can stabilize and support itself. Otherwise, the relief offered by probiotics will simply be an additional temporary remedy to our ailments. A probiotic craze among healthy individuals will only prolong the inevitable realization that supplementing a healthy microbiome is not as sustainable as establishing a healthy microbiome through diet. On the other hand, the use of probiotics as a therapy to improve the mental state of those suffering from mood disorders could be a step in the right direction to establishing more knowledge about the gut-brain axis and to what extent it controls our behavior.
Further reading
An additional study that showed similar benefits of probiotic intervention for improving mood:
- Messaoudi, M., Violle, N., Bisson, J.F., Desor, D., Javelot, H., Rougeot, C. (2011). Beneficial psychological effects of a probiotic formulation (Lactobacillus helveticus R0052 and Bifidobacterium longum R0175) in healthy human volunteers. Gut Microbes 2 (4), 256—261. https://dx.doi.org/10.4161/gmic.2.4.16108
This paper provides a good description of the brain-gut axis and its function:
- Dinan, T. G., Stilling, R. M., Stanton, C., & Cryan, J. F. (2015). Collective unconscious: How gut microbes shape human behavior. Journal of Psychiatric Research, 63, 1—9. https://dx.doi.org/10.1016/j.jpsychires.2015.02.021
This TED talk provides a great introduction to the gut-brain axis
Focal Paper
Steenbergen, L., Sellaro, R., van Hemert, S., Bosch, J. A., & Colzato, L. S. (2015). A randomized controlled trial to test the effect of multispecies probiotics on cognitive reactivity to sad mood. Brain, Behavior, and Immunity, 48, 258—264. https://doi.org/10.1016/j.bbi.2015.04.003
References
Benton, D., Williams, C., Brown, A. (2006). Impact of consuming a milk drink containing a probiotic on mood and cognition. Eur. J. Clin. Nutr. 61 (3), 355—361.https://dx.doi.org/10.1038/sj.ejcn.1602546
Bravo, J.A., Forsythe, P., Chew, M.V., Escaravage, E., Savignac, H.M., Dinan, T.G., Cryan, J.F. (2011). Ingestion of Lactobacillus strain regulates emotional behavior and central GABA receptor expression in a mouse via the vagus nerve. Proc. Natl. Acad. Sci. 108 (38), 16050—16055. https://dx.doi.org/10.1073/pnas.1102999108
Desbonnet, L., Garrett, L., Clarke, G., Kiely, B., Cryan, J.F., Dinan, T.G. (2010). Effects of the probiotic Bifidobacterium infantis in the maternal separation model of depression. Neuroscience, 170 (4), 1179—1188. https://dx.doi.org/10.1016/j. neuroscience.2010.08.005.
Dinan, T. G., Stilling, R. M., Stanton, C., & Cryan, J. F. (2015). Collective unconscious: How gut microbes shape human behavior. Journal of Psychiatric Research, 63, 1—9. https://dx.doi.org/10.1016/j.jpsychires.2015.02.021
Dinan, T. G., & Cryan, J. F. (2016). Mood by microbe: towards clinical translation. Genome Medicine, 8(1), 36. https://doi.org/10.1186/s13073-016-0292-1
Kang, S. S., Jeraldo, P. R., Kurti, A., Miller, M. E., Cook, M. D., Whitlock, K., Goldenfeld, N., Woods, J.A., White, B.A., Chia, N., Fryer, J.D. (2014). Diet and exercise orthogonally alter the gut microbiome and reveal independent associations with anxiety and cognition. Molecular Neurodegeneration, 9(1), 36. https://doi.org/10.1186/1750-1326-9-36
Messaoudi, M., Violle, N., Bisson, J.F., Desor, D., Javelot, H., Rougeot, C. (2011). Beneficial psychological effects of a probiotic formulation (Lactobacillus helveticus R0052 and Bifidobacterium longum R0175) in healthy human volunteers. Gut Microbes, 2 (4), 256—261. https://dx.doi.org/10.4161/gmic.2.4.16108
Rao, A.V., Bested, A.C., Beaulne, T.M., Katzman, M.A., Iorio, C., Berardi, J.M., Logan, A.C. (2009). A randomized, double-blind, placebo-controlled pilot study of a probiotic in emotional symptoms of chronic fatigue syndrome. Gut Pathog. 1 (1), 1—6. https://dx.doi.org/10.1186/1757-4749-1-6
