Background
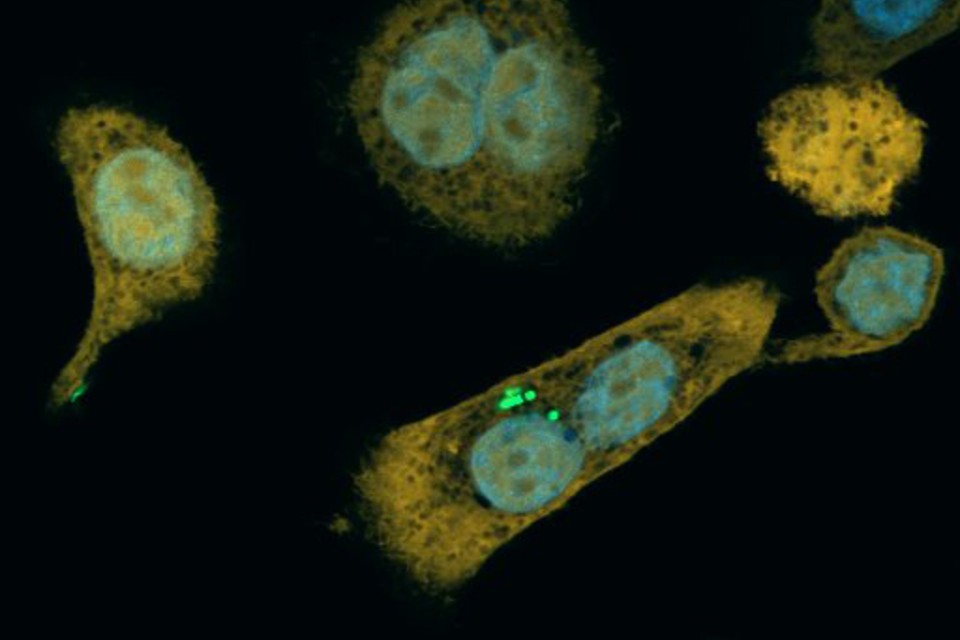
The Yanomami people are patches of isolated South American tribes who occupy mountainous regions of southern Venezuela. Recently, a Yanomami tribe of 34 subjects discovered by helicopter, was investigated by a team of researchers who accompanied medical care professionals who were providing care to the villagers. These researchers, Clemente et. al. (2015), then wrote the paper, “The microbiome of uncontacted Amerindians’ to analyze this population which was uniquely untouched by Western Society. An interesting topic that this research paper addresses is antibiotic-resistant bacteria. Antibiotic-resistance are the adaptations of a bacterial species in response to antibiotics. Antibiotics are medications that have been developed in more recent times to destroy bacteria cells but not human cells. They do this by targeting specific differences between the two types of cells, for instance, penicillin inhibits the synthesis of the peptidoglycan layer of bacterial cell walls a feature not present in animal cells. Other bacteria have distinct DNA replication processes and some antibiotics are able to interrupt that function as well. This Yanomami population is intriguing because their microbiomes are likely the most accurate representation of an ancient human microbiome due to their isolation from the Western world. The presence of antibiotic-resistant bacteria in the Yanomami gut provides evidence for the claim that antibiotic-resistant bacteria have been around since before the invention of antibiotics, so stay tuned for a persuasive evidentiary argument further down. Clemente et. al. also state that the Yanomami population that is sampled is the most diverse microbiome ever recorded. It is important to understand what kind of diversity the researchers are talking about. The Yanomami show extremely high beta diversity when compared to Guahibo, Malawi, and U.S. populations but exhibit low alpha diversity amongst individuals in the village population. Beta diversity represents the differences in species composition among samples while alpha diversity is just the diversity of each sample. This means that the Yanomami microbiome sample is extremely unique but microbiomes within that sample are very similar, this is most likely due to the Yanomami leading vastly different lifestyles than Western societies and individuals in the village being in extremely close quarters with each other (eating the same food, drinking from the same water source, no waste removal, etc.). Continue reading “Which came first, antibiotics, or antibiotic-resistance? A study of Uncontacted Amerindians.”